Breast Cancer Awareness Month – Wear It Pink Day

During Breast Cancer Awareness Month and on Wear It Pink day we’d like to share one of our own team member’s personal journey with her second breast cancer diagnosis.
’Shortly, in fact just a matter of three weeks, after our Pink Ladies photo was taken on last year’s Wear It Pink Day I was diagnosed with my second occurrence of breast cancer – this time in the other breast.
It had been 14 years since my last battle so it came as a bit of a shock.
I regularly check myself, and my husband Marc ensures I go every year for a mammogram and MRI, but I didn’t feel these two lesions as they were deep down behind the nipple. One lesion was around 10mm and the other a little smaller – both having grown in a year.
Strangely I felt calm – I’d been and done it before and had the best and, fortunately, the same team seeing me through the process again. Mr Stacey-Clear, my consultant surgeon, just has the most amazing calming effect and I had/have the utmost confidence in him.
The worst part for me was the feeling I was letting down my family and friends by putting them through this worry all over again. I hated this.
Mr Stacey-Clear made a plan for surgery and was able to arrange for me to be in the hands of the same Oncologist, Professor Ian Smith, at The Royal Marsden (Sutton).
We started with a lumpectomy and lymph node extraction on the 7th December 2021. Gown and lovely DVT socks on, I started with a procedure via ultrasound to insert some surgical guide lines to help with the surgery – I had previously had titanium clips put in when the biopsies had been taken. Surgery was in the afternoon but I was tucked up in my own bed that evening.
A little while after the results were back and for the second time I had Triple Negative Breast Cancer (invasive ductal carcinoma grade 3). The bonus was that it hadn’t spread to the lymph nodes.
Mr Stacey-Clear recommended that I undergo genetic testing this time. I had been 39 the first time round, and was now 53 (still relatively young by my standards), having been diagnosed twice with the same type of breast cancer. More importantly I had a 19 year old daughter, Maisie, and I needed to know if a breast cancer gene had been passed onto her so she could take the necessary precautionary measures in the future.
I met with the Oncologist before Christmas and he scheduled a chemo plan to start on 13th January 2022. He also arranged for me to have a port fitted in my chest to enable bloods to be drawn and the Paclitaxel chemo drugs to be administered.
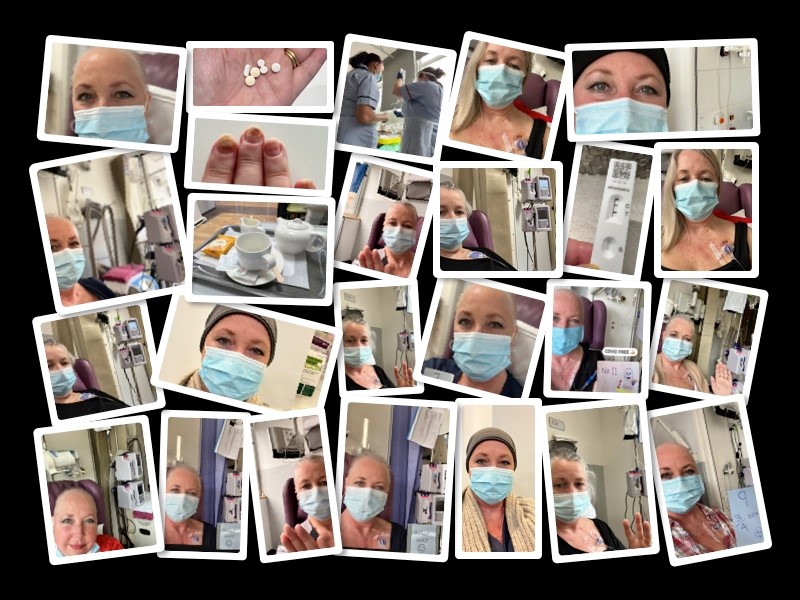
Now this is when I realised the advances breast cancer research had made into treatment – supported greatly by charities like Breast Cancer Now.
14 years ago I underwent six chemo sessions – one every three weeks – and at each session a nurse had to slowly and carefully inject the chemo by hand as it was so toxic. This time I was scheduled 12 sessions – one a week – and I was connected to a machine that slowly administered the chemo. Research had shown that this new programme had the same effect and the bonus is that it keeps the treatment time to a minimum.
Karen, my Breast Clinical Nurse Specialist, went through the side-effects. Hair loss is one that most would worry about and the use of scalp cooling can reduce or stop hair loss all together. I had experience of scalp cooling before and to be honest it wasn’t overly successful so I decided to go without – whatever the consequence. Marc was very supportive of my decision even though he would have to look at me daily.
Before chemo started my pathology results were in from the surgery and the genetic tests were complete. Unfortunately the margin taken around the lesions still indicated some active cells so I would need to go back in for more surgery once the chemo plan was complete.
On the plus side though, my genetic tests for BRCA1 & 2, PALB2, CHEK2 and ATM genes were all clear. I was so relieved for Maisie and so pleased that she now qualifies for screening from the age of 40. Of course I’ll be on at her to check her-self regularly – recommended from her mid to late 20s.
13th January 2022, day one of my treatment, started with me arriving at The Royal Marsden at 7:30am to prepare for my port insertion followed by my first chemo session.
Parking at The RM is a little challenging so Marc drove me to every appointment, dropped me off and went off to work to wait for me as he wasn’t allowed into the hospital due to COVID worries. I have to say that although completely understandable, not being able to come in for my appointments and chemo sessions was very hard for him – he missed not being able to support me but he doesn’t realise what he was doing was just that.
The procedure to insert the port was performed whilst I was awake. The surgeons gave me a little bit of sleepy stuff, and local numbing, but I was able to talk and hear them whilst feeling nothing. That afternoon I was moved to the chemotherapy ward. The Medical Practitioner sat down with me to explain what was about to happen. There was mention of a possible allergic reaction (although medication would be given to minimise this before the session) and not to be alarmed if I would suddenly see a team of 8-10 people around me. Not ever having had an allergic reaction I pushed this information to one side as it was only ‘possible’.
How wrong I was, within 20 seconds of my first session I had a reaction like I’ve never felt before. Meanwhile the Nurse keeping an eye on me raised the alarm and there they were the 8-10 people stood in front of me. Oh they were so calm – helping me to stay clam and enabling me to answer their questions. I was taken off the chemo and given some medication to reduce the allergy reactions I was feeling. I was rested for about an hour and then we restarted again – no effects this time. It was an 11 hour day that day but I was so glad I was underway with my treatment. As a result of my initial reaction I was given a bundle of medication to take the day before, day of and day after my chemo sessions – I didn’t react again.
Every week, the day before chemo, I would go for my blood tests to check my levels and suitability to continue with the chemo, and I would meet with a Medical Practitioner to discuss how I was feeling. The one thing I have learnt is to be totally honest about how you are feeling – whether you have constipation, acid reflux, tiredness, discoloured nails, nausea, tingling in your fingers or feet, don’t be embarrassed or worried about mentioning it. They’ve heard it all before and in many cases are able to adjust or prescribe additional medication to help with the symptoms, or simply give you advice on foods to avoid or changes you can make to your lifestyle. Don’t be shy, speak out.

Every week I was greeted by the most wonderful people at The Royal Marsden – from the volunteers at the entrance doors, the reception teams, the ladies that took my bloods, the practitioners and consultants, through to the nurses in the chemo wards. They are just amazing!
I quite enjoyed my chemo sessions – a chat with the nurses, a cup of tea with a biscuit and general people watching. As COVID was rife I had kept myself quite isolated trying to avoid it – unfortunately I was to succumb just two weeks before the end of my chemo treatment plan. Fortunately this wasn’t a problem and I was able to continue as soon as I tested COVID negative with the last two sessions.
My hair journey started with a bit of hair-loss after about two weeks. I had longish hair and after a gentle wash my loose hair decided to tangle itself into a huge hair ball at the back of my head. Mum was with me so I asked her to take the kitchen scissors and cut it out – telling her not to worry about what it looked like as I had ordered a wide range of hats. Later that day my friend and hairdresser Katy came to the house to do what she could in creating a hairstyle of sorts. She was back a few days later, as I’d lost more and it was looking bad, to give me a crewcut with the clippers. I wasn’t sad or down in the dumps and I quite looked forward to the simplicity of looking after very short hair. I was told I ‘rocked’ the new look – so very kind of them to say.
By the beginning of March I looked like a balding hedgehog so I decided it was time for the full shave off. Marc had already purchased, some time ago, some clippers and a fresh razor blade so he was very keen to use them. We did laugh and we could make a barber of him yet. Apparently I have a very good shaped head for baldness which is always a bonus. What helped with the look was that I did keep my eyebrows and eyelashes till a few weeks after chemo – after then I had to make a bit more effort with the make-up. Oddly, and even though I was still having chemo, my hair started to grow back almost immediately – slowly thickening up.
I did have other chemo side-effects. The nails on both my hands and feet turned black – thank goodness for breathable nail varnish as gel nail polish is not recommended. I started to get a tingling in my hands and feet so they adjusted my chemo for the last couple of weeks in order to avoid this becoming a longterm problem (it worked!). A two stone weight gain which I know I’ll work off slowly. Moon face, yes it’s a proper term, making my face look very round but again this has, I think, lessened a lot. Stomach issues resulting in constipation and acid reflux – both treated by added medication and dietary changes. I only ever had one day of nausea – again I had tablets for this. Of course there was the odd day of tiredness but I tried to get out with the dogs whenever I could even if it meant pushing myself to leave the house to get some fresh air.
My last chemo session was on the 14th April and after 12 days rest I was back in for further surgery to remove more tissue. The active cells are all gone now.

After a week’s recovery I met with my Radiotherapist, Dr Tait, whom had been my Radiotherapist last time. We discussed my treatment plan, possible side effects and what would happen next.
Once again I was amazed to hear how research had reduced what had been a six and a half week (every day except weekends) radiotherapy programme to just one week of targeted radiotherapy and, as I had had a reoccurrence of Triple Negative Breast Cancer, I was scheduled another week targeted at the whole breast. 33 days down to 10 with no significant change in side-effects but with the right outcome.
I went for a planning scan on the 5th May and treatment started on 19th May. As I already had little pinprick tattoos from the last time they were able to use them again to line up the machine. I did experience a couple of side-effects – a warm sensation in the treated area and a very annoying prickle heat rash. The nurses were great and were able to suggest the right cream to keep the area moisturised and Dr Tait recommended the right cream for the rash.
I finally completed my treatment on the 1st June 2022 and am well on my way to a full recovery. My next check up scans are in November and I have a good feeling about the results.
I couldn’t have got through this last year without the support of my family, friends, colleagues (particularly the Pink Ladies), and hospital teams – you are all heaven sent!
On a final note… if you are offered a mammogram then book an appointment and make sure you go. Check yourself regularly and if you find anything unusual make an appointment to see your doctor. The earlier breast cancer is detected the more likely it can be treated with a positive outcome.’


